The recent passing of a 48-year-old actor has once again drawn attention to a troubling trend: colorectal cancer is affecting younger people more often than before. While overall cancer death rates among individuals under 50 have fallen significantly since 1990, colorectal cancer has moved in the opposite direction. Today, it has become the leading cause of cancer-related deaths in adults under 50. This disease develops in the colon or rectum and often progresses quietly over time.
Experts warn that the rise in cases among younger adults is unlikely to slow down anytime soon. Although most diagnoses still occur after age 50, the number of cases in people in their 20s, 30s, and 40s has increased steadily over the past few decades.
Screening Guidelines: Why Age 45 Matters
When should you begin screening for colorectal cancer?
Health authorities, including federal agencies and the American Cancer Society, recommend that adults at average risk start screening at age 45. The most common options include:
A colonoscopy every 10 years
Stool-based tests every one to three years
Insurance coverage for preventive screening is typically based on these guidelines.
Screening begins at 45 because colorectal cancer usually develops slowly. It often starts as small growths called polyps, which can take years to become cancerous. Detecting and removing these growths early can prevent cancer altogether.
The recommended starting age was lowered from 50 to 45 after research showed a noticeable increase in risk beginning in the mid-40s. For example, the risk more than doubles between ages 40–44 and 45–49.
Even so, experts emphasize that while rates are rising among younger adults, the overall risk before age 50 remains relatively low.
Why Not Screen Everyone Earlier?
Creating screening guidelines is complex. Researchers must balance the benefits of early detection against potential risks, costs, and healthcare capacity. There are only so many specialists available to perform colonoscopies, and even now, many patients wait months for an appointment.
Another challenge is participation. Only about one in five eligible adults aged 45–49 are currently up to date with screening. Expanding screening to even younger groups could further strain resources while participation rates remain low.
Who Should Start Screening Earlier?
Some people should not wait until 45. Earlier screening is recommended if you have:
A family history of colorectal cancer
A personal history of polyps or colorectal disease
Close relatives diagnosed at a young age
Even a noncancerous polyp in a parent at an early age may mean you should begin screening sooner. It’s important to discuss your family medical history with a healthcare provider.
If symptoms are already present, the test is considered diagnostic rather than preventive, and insurance may cover it regardless of age.
Early Warning Signs You Shouldn’t Ignore
Colorectal cancer symptoms can appear months or even years before diagnosis. Key warning signs include:
Persistent abdominal pain
Rectal bleeding
Ongoing diarrhea or changes in bowel habits
Iron-deficiency anemia or unexplained low red blood cell counts
Because these symptoms can resemble common digestive issues, they are often overlooked. However, if symptoms persist or occur together, medical evaluation is essential.
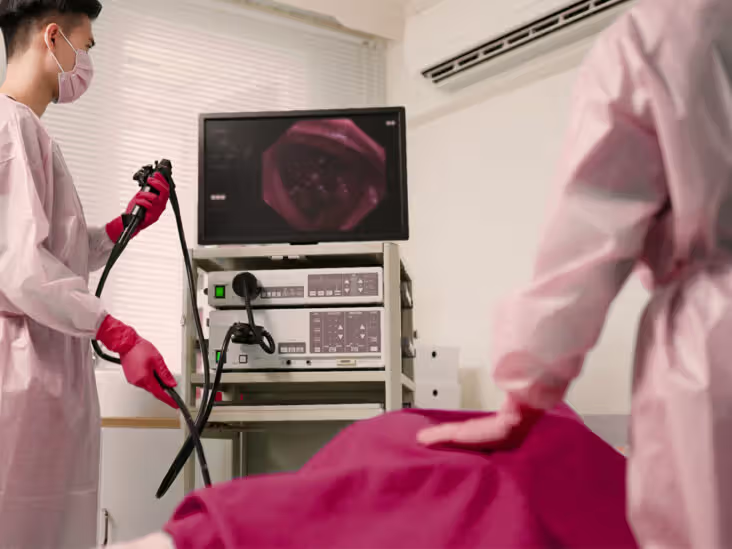
Screening Options: Colonoscopy vs. At-Home Tests
Colonoscopy remains the gold standard because it can both detect cancer and remove precancerous polyps in one procedure.
Noninvasive options approved by the FDA include:
Stool DNA tests (such as Cologuard)
Fecal immunochemical tests (FIT)
Blood-based screening tests
These tests are effective at detecting cancer but are less reliable at finding precancerous polyps. If any of them show abnormal results, a follow-up colonoscopy is required.
For people under 45 without risk factors, insurance may not cover screening. Out-of-pocket costs for a colonoscopy typically range from about $1,250 to more than $4,000.
Why Cases Are Rising in Younger People
Researchers are still investigating the causes, but several factors may be contributing:
Increasing obesity rates
Lower physical activity
Diets high in ultraprocessed foods
Changes in gut bacteria
Possible links to antibiotic use
While screening is critical, lifestyle changes can also play a major role in prevention. Maintaining a healthy weight, exercising regularly, and improving diet quality have been shown to reduce colorectal cancer risk.
The Bottom Line
When should you begin screening for colorectal cancer?
For most adults at average risk, screening should start at age 45. However, anyone with symptoms, a family history, or other risk factors should speak with a doctor about earlier testing. Early detection saves lives—and combining screening with healthy lifestyle choices offers the best protection against this increasingly common cancer.

